

Medical debt has deep historical roots, evolving from personal obligation and community negotiation into modern systems of billing, insurance, and institutional enforcement.

By Matthew A. McIntosh
Public Historian
Brewminate
Introduction: Healing and Obligation in Historical Context
Medical care has never existed outside the structures of obligation, exchange, and economic reality, even in its earliest recorded forms. From ancient societies to the early modern period, healing was embedded within systems of reciprocity, status, and material compensation. Physicians, healers, and caregivers operated within economies that demanded payment, whether in coin, goods, or social capital, and their work was shaped by these expectations. The act of healing carried ethical weight, often framed as a duty to preserve life rather than a purely transactional service. This tension between moral obligation and economic necessity forms the foundation for understanding medical debt in the premodern world.
Unlike modern healthcare systems, which rely on institutional frameworks such as insurance and standardized billing, premodern medicine functioned within decentralized and highly variable systems of payment. Fees were often negotiated directly between practitioner and patient, with little uniformity across regions or social classes. In many cases, the ability to pay determined not only the cost of care but also the quality and accessibility of treatment. Wealthier individuals could secure the services of highly trained physicians, while poorer populations relied on informal care, charity, or delayed payment arrangements. These disparities reveal that economic stratification has long shaped medical access, even in societies that emphasized the ethical duties of healers.
Medical debt in the premodern world cannot be understood solely through the lens of formal economic systems. It was deeply intertwined with social relationships, community expectations, and reputational dynamics. Physicians often depended on long-term relationships with patients and communities, balancing the need to sustain their livelihoods with the expectation that they would provide care regardless of immediate payment. This created a system in which debts were not always enforced through legal mechanisms but were instead managed through trust, obligation, and social pressure. Such arrangements allowed for flexibility but also introduced uncertainty, as practitioners bore the risk of nonpayment in exchange for maintaining their standing within the community.
The historical development of medical debt reflects a broader and enduring tension between the ideals of care and the realities of compensation. Across different societies and periods, this tension manifested in various forms, from formalized debt systems in ancient civilizations to informal, negotiated arrangements in later periods. Understanding these dynamics provides essential context for examining how medical debt was managed, enforced, or avoided before the rise of modern financial and institutional structures. It also highlights the continuity of a problem that remains deeply relevant, as the balance between healing and obligation continues to shape healthcare systems in the present.
Ancient Foundations: Debt, Law, and Enforcement in Early Civilizations

The origins of medical debt must be situated within the broader legal and economic frameworks of early civilizations, where obligations for goods and services were rigorously defined and enforced. In societies such as ancient Mesopotamia and Rome, debt was not an informal or purely personal matter but a structured legal relationship governed by codified rules. These systems did not distinguish sharply between different types of debt, meaning that obligations incurred for medical treatment were embedded within the same mechanisms that governed loans, labor, and property. The enforcement of medical debt was shaped by legal traditions that emphasized repayment, accountability, and, in some cases, severe penalties for default.
In Mesopotamia, one of the earliest known legal systems, debt regulation was articulated through codes such as the Code of Hammurabi, which established clear expectations regarding contracts, compensation, and liability. While specific provisions for medical services focused primarily on malpractice and physician fees, they reveal a broader context in which economic exchange was closely monitored and enforced by the state. The code set standardized fees for certain procedures based on the social status of the patient, demonstrating that medical care was already integrated into a structured system of economic valuation. The legal framework imposed strict penalties for failure, indicating that both practitioners and patients operated within a system of defined risk and obligation. Debtors who failed to meet their obligations could face significant consequences, including the forfeiture of property, the seizure of goods, or even temporary debt servitude, in which individuals or their family members were compelled to work off obligations. These measures underscore the seriousness with which financial obligations were treated and highlight the potential risks faced by individuals who incurred debts, including those related to medical care, within a system that prioritized enforceability and order.
The Roman world developed even more elaborate systems of debt enforcement, integrating legal, social, and economic mechanisms to ensure repayment. Roman law provided creditors with substantial authority, allowing them to pursue debts through courts and, in earlier periods, through forms of personal coercion. Although practices such as debt bondage evolved, the underlying principle remained that obligations were binding and enforceable. Physicians operating within this system were not exempt from its constraints, and their ability to collect payment depended on the same legal frameworks that governed other forms of debt. This integration of medical services into the broader economic system reflects the normalization of healthcare as a compensable, and enforceable, transaction.
The enforcement of debt in these societies was not solely a matter of legal procedure but was also influenced by social hierarchy and status. Elite individuals often possessed greater flexibility in managing debts, whether through negotiation, patronage, or access to legal resources, while those of lower status faced harsher consequences for nonpayment. This disparity extended to medical care, where wealthier patients could secure treatment with the expectation of payment, while poorer individuals risked incurring obligations that they might struggle to fulfill. This meant that the burden of enforcement fell disproportionately on those least able to absorb it, reinforcing existing social inequalities through legal mechanisms. The intersection of law and social structure played a critical role in shaping how medical debt was experienced and enforced across different segments of society, embedding economic vulnerability within the very systems designed to regulate obligation.
The systems of debt in ancient civilizations demonstrate that medical obligations were deeply embedded within formal legal and economic institutions. Far from being an exceptional category, medical debt was subject to the same principles of enforcement that governed other forms of financial obligation. These early frameworks established a precedent for understanding healthcare as both a moral service and an economic transaction, a duality that would continue to shape medical practice in later periods. By examining these foundations, it becomes clear that the challenges associated with medical debt have long been intertwined with broader questions of law, equity, and social order.
Medicine and Payment in Classical Antiquity

In classical antiquity, the practice of medicine operated within a complex intersection of professional identity, social status, and economic exchange. Physicians in the Greek and Roman worlds were not part of a centralized or regulated system of payment but instead negotiated compensation directly with patients. This created a flexible yet uncertain environment in which fees could vary widely depending on the practitioner’s reputation, the patient’s wealth, and the nature of the illness. While medicine was often framed as a learned and even noble pursuit, it remained firmly embedded within systems of economic transaction, where healing was expected to be compensated.
In the Greek world, physicians frequently established their reputations through both skill and public demonstration, attracting patients who could afford their services. The Hippocratic tradition, while emphasizing ethical conduct and professional responsibility, did not eliminate the expectation of payment. Instead, it acknowledged the practical realities of medical practice, advising physicians to consider the financial circumstances of their patients when determining fees. This guidance reflects an early recognition of the tension between ethical obligation and economic necessity, as practitioners were encouraged to balance their duty to heal with the need to sustain their livelihoods. Such flexibility allowed physicians to maintain their professional standing while adapting to the varied economic conditions of their communities.
Roman medicine further illustrates the integration of healthcare into broader social and economic systems, particularly through the role of patronage and social hierarchy. Elite physicians often secured the support of wealthy patrons, who provided financial stability in exchange for ongoing medical service and social prestige. This arrangement reduced the need for direct fee collection while reinforcing the connection between medical care and social status. Physicians who lacked such patronage relied on more conventional forms of payment, navigating a competitive environment in which reputation and success were closely tied to economic outcomes.
Despite these structures, the collection of medical fees in classical antiquity was not always straightforward. Physicians faced challenges in securing payment, particularly from patients of lower economic status or in situations where outcomes were uncertain. Unlike other forms of debt, medical payment could be complicated by the unpredictable nature of treatment, where success was not guaranteed. This uncertainty sometimes led to disputes over fees, with patients reluctant to pay for unsuccessful treatments and physicians seeking to assert the value of their expertise regardless of outcome. In some cases, payment arrangements may have been negotiated in advance, while in others they were determined after the fact, further complicating expectations on both sides. These dynamics created an environment in which trust, reputation, and ongoing relationships were essential to sustaining medical practice, as formal enforcement mechanisms were often limited or socially undesirable. Such tensions highlight the precarious position of medical practitioners within a system that valued both results and reputation while offering few guarantees of consistent compensation.
The economic realities of medical practice also contributed to a degree of stratification within the profession itself. Highly trained and well-regarded physicians could command substantial fees and attract elite clientele, while less prestigious practitioners, including itinerant healers and specialists, often worked for lower compensation. This internal hierarchy mirrored the broader social divisions of classical societies, reinforcing the idea that access to quality medical care was closely tied to wealth and status. Payment for medical services functioned not only as an economic transaction but also as a marker of social distinction.
Medicine in classical antiquity reveals a system in which healing and payment were deeply intertwined, shaped by both ethical ideals and practical constraints. Physicians navigated a landscape defined by negotiation, reputation, and social relationships, balancing their roles as caregivers and economic actors. The challenges associated with collecting fees, managing expectations, and maintaining professional standing underscore the enduring complexity of medical debt as a historical phenomenon. These dynamics provide important context for understanding how later societies would continue to grapple with the relationship between care, cost, and obligation.
Medieval Practice: Community, Charity, and Informal Enforcement

Medical practice in the medieval world was shaped less by formal systems of billing and enforcement than by community relationships, religious obligation, and localized economic exchange. Unlike the more codified legal structures of antiquity, medieval societies often relied on informal arrangements to manage payment for care. Physicians, surgeons, and healers operated within social networks where reputation and trust played central roles, and where the expectation of compensation was balanced against moral and religious duties to provide care. Medical debt existed but was rarely enforced through rigid legal mechanisms, instead taking on a more flexible and negotiated character.
One of the most significant influences on medieval medical practice was the role of the Church and charitable institutions. Monasteries, hospitals, and religious foundations provided care to the sick and poor, often without direct payment. These institutions framed healing as an act of charity and spiritual duty, emphasizing the care of the body as part of a broader concern for the soul. The growth of hospitals in the later medieval period, particularly in urban centers, reflects an increasing institutionalization of this charitable model, though these facilities often prioritized spiritual care, rest, and basic sustenance over advanced medical treatment. Patients were frequently expected to participate in religious observances such as confession and prayer, reinforcing the idea that illness had both physical and spiritual dimensions. Many individuals who could not afford medical services relied on these institutions, reducing the need for formal debt collection in certain contexts. This system did not eliminate economic considerations entirely, as such institutions themselves depended on donations, endowments, and patronage to sustain their operations, creating an indirect but persistent link between care and financial support.
Outside of charitable settings, medical practitioners frequently negotiated fees directly with patients, adapting their expectations based on the individual’s social and economic circumstances. Payment might be delayed, reduced, or substituted with goods and services, reflecting the limited availability of coinage in many regions. This flexibility allowed physicians to maintain relationships within their communities while ensuring some level of compensation for their work. It introduced uncertainty, as practitioners often bore the risk of nonpayment in exchange for preserving their reputation and social standing.
Informal enforcement mechanisms played a crucial role in managing medical debt. Rather than relying on courts or legal sanctions, practitioners often depended on social pressure, reputation, and community expectations to secure payment. A patient who failed to honor obligations risked damaging their standing within the community, which could have broader social and economic consequences, including exclusion from local networks of support and exchange. Similarly, physicians who were perceived as overly aggressive in pursuing payment risked alienating potential patients and undermining their professional reputation, which was essential for sustaining their practice. In some cases, long-term relationships allowed debts to be carried over extended periods, with repayment occurring gradually or through reciprocal services rather than immediate settlement. These dynamics created a delicate balance in which both parties were constrained by shared norms and expectations, ensuring that enforcement remained embedded within the fabric of community life rather than external legal systems.
The structure of medieval society also reinforced disparities in access to care and the management of medical debt. Wealthier individuals could secure the services of trained physicians and were more likely to fulfill payment obligations, while poorer populations relied on a combination of charity, informal care, and delayed payment arrangements. In some cases, local healers or “wise women” provided treatment without formal fees, operating within traditions of communal support rather than market exchange. This stratification highlights the ways in which economic and social hierarchies shaped not only access to care but also the mechanisms through which medical obligations were managed.
Medieval medical practice reveals a system in which economic exchange, social obligation, and ethical considerations were deeply intertwined. Medical debt existed as a persistent feature of this system, but its management depended less on formal enforcement than on relationships, reputation, and community norms. This approach allowed for a degree of flexibility that could accommodate the varied circumstances of patients, but it also placed significant burdens on practitioners, who often navigated uncertain and inconsistent systems of compensation. The medieval experience represents a distinct phase in the history of medical debt, one in which informal enforcement and moral economy played a central role.
Early Modern Developments: Regulation, Fees, and Patient Protection

The early modern period marked a transitional phase in the history of medical debt, as emerging state structures and professional identities began to shape the regulation of medical practice and payment. While informal systems of negotiation and community-based enforcement persisted, there was a growing recognition that medical fees required some degree of oversight. This shift reflected broader developments in governance and legal authority, as states increasingly sought to regulate economic activity, including the provision of medical services. Within this evolving framework, the relationship between physician and patient became more structured, though it remained far from standardized.
One of the key developments of this period was the introduction of legal measures designed to regulate medical fees and protect patients from excessive charges. In some regions, including parts of colonial North America, laws were enacted to limit the amounts that physicians could charge for their services. These regulations were often motivated by concerns that medical practitioners might exploit their specialized knowledge to impose unreasonable costs on patients. By establishing limits or guidelines for fees, authorities sought to balance the economic interests of physicians with the need to ensure fair access to care. These laws reflected broader anxieties about professional authority and the potential for abuse within emerging medical markets, where patients often lacked the expertise to evaluate the necessity or value of treatments. Such measures highlight the growing awareness of the potential for conflict between professional autonomy and public welfare, as well as the increasing willingness of governing bodies to intervene in the relationship between doctor and patient.
The professionalization of medicine contributed to changes in how payment was structured and perceived. As physicians increasingly sought formal training and credentials, they also asserted their status as skilled professionals entitled to appropriate compensation. This shift reinforced the idea that medical services carried a measurable economic value, distinct from purely charitable or informal care. The lack of centralized billing systems meant that fees were still often negotiated on a case-by-case basis, leaving significant room for variation and dispute. The emerging professional identity of physicians coexisted with older practices of negotiation and flexibility.
Disputes over medical fees became more visible during this period, reflecting both the increasing formalization of practice and the persistence of economic uncertainty. Physicians occasionally turned to legal mechanisms to recover unpaid debts, though such actions were often complicated by social expectations and reputational concerns. Pursuing payment through the courts could damage a practitioner’s standing within the community, particularly if it was perceived as overly aggressive or contrary to the ethical ideals of the profession. In some instances, disputes centered not only on whether payment was owed but also on the appropriate valuation of medical services, especially in cases where outcomes were uncertain or unsuccessful. Patients might contest fees on the grounds that treatment had failed, while physicians argued for compensation based on effort and expertise rather than results. These conflicts reveal the inherent ambiguity in pricing medical care and underscore the challenges of enforcing payment in a context where both ethical considerations and practical realities shaped expectations.
The tension between regulation and autonomy also shaped the broader landscape of medical debt in the early modern world. While laws sought to protect patients, they could also limit the ability of physicians to secure adequate compensation, particularly in regions where economic conditions were unstable. Practitioners had to navigate a complex environment in which their fees were subject to scrutiny, yet their livelihoods depended on the willingness and ability of patients to pay. This balancing act reflects the continued interplay between economic necessity and ethical obligation, a dynamic that remained central to medical practice.
The early modern period represents a stage in which medical debt became more visible as a subject of legal and social concern, without yet being fully institutionalized. The introduction of regulation, combined with the ongoing importance of informal arrangements, created a hybrid system in which multiple approaches to payment and enforcement coexisted. This transitional character underscores the gradual nature of change in medical economics, as older practices adapted to new legal and professional frameworks. By examining these developments, it becomes clear that the management of medical debt continued to evolve in response to shifting expectations about fairness, responsibility, and the role of the state.
The Eighteenth and Nineteenth Centuries: Physician Struggles with Payment

The eighteenth and nineteenth centuries marked a period in which the challenges of collecting medical payment became increasingly visible and widely discussed among practitioners. As medical practice expanded and professional identity became more defined, physicians found themselves operating within economies that relied heavily on credit and delayed payment. Unlike modern systems with structured billing and enforcement mechanisms, physicians often extended care with the expectation that payment would be made at a later date, if at all. This system created a persistent tension between the provision of care and the uncertainty of compensation, leaving many practitioners financially vulnerable despite their professional status.
Account books from this period provide valuable insight into the realities of medical practice, revealing long lists of unpaid or partially paid bills. Physicians carefully recorded visits, treatments, and fees, yet these records often reflected debts that remained outstanding for months or even years. In many cases, patients lacked the immediate means to pay, particularly in rural or economically unstable regions where cash was scarce. Physicians were drawn into extended financial relationships with their patients, in which payment depended on future harvests, business success, or other unpredictable factors. These records also demonstrate the routine nature of partial payments, where small amounts were paid intermittently over time rather than in full, further complicating financial accounting. In some instances, debts were carried across generations, with family members assuming responsibility for outstanding balances, illustrating the deeply embedded nature of credit within local economies. These conditions highlight the extent to which medical practice was intertwined with broader patterns of credit and economic fluctuation, leaving physicians dependent on forces beyond their control.
The reliance on credit-based systems also exposed physicians to significant financial risk, as there were limited means of enforcing payment without damaging professional relationships. While legal avenues for debt recovery existed, many practitioners were reluctant to pursue them, fearing that such actions would harm their reputation within the community. A physician who gained a reputation for aggressively collecting debts risked losing patients, particularly in smaller communities where personal relationships were central to professional success. This reluctance to enforce payment formally contributed to a cycle in which unpaid debts accumulated, further complicating the economic stability of medical practice.
Professional discourse during this period reflects widespread frustration among physicians regarding the difficulty of securing payment for their services. Medical journals, personal correspondence, and professional writings frequently include complaints about patients who delayed or avoided payment altogether. These discussions reveal a growing awareness of the economic challenges inherent in medical practice, as well as a sense that the profession was undervalued despite its importance. Physicians often framed these issues in moral as well as economic terms, expressing concern that patients failed to appreciate the skill and effort involved in medical care. Some practitioners argued for greater professional solidarity or the establishment of standardized fee structures, though such proposals were difficult to implement in decentralized and competitive markets. These debates illustrate an ongoing struggle to reconcile the ideals of professional dignity with the realities of inconsistent and often unreliable compensation.
Physicians developed adaptive strategies to manage these challenges, often tailoring their practices to the economic realities of their communities. Sliding-scale fees, barter arrangements, and selective forgiveness of debts became common, allowing practitioners to maintain relationships while mitigating financial losses. In many cases, payment took non-monetary forms, including goods, labor, or services, reflecting the limited circulation of cash in certain regions. These arrangements allowed physicians to sustain their practices while accommodating the needs of their patients, but they also introduced additional complexity into the management of accounts and obligations. The decision to forgive or reduce a debt was often influenced by considerations of reputation, charity, and long-term relationships, rather than purely economic calculation. While these strategies provided a degree of flexibility, they did not eliminate the underlying problem of inconsistent payment, and many practitioners continued to face significant financial uncertainty.
The struggles of physicians in the eighteenth and nineteenth centuries underscore the persistent difficulty of reconciling medical care with reliable compensation. The absence of standardized systems for billing and collection placed the burden of financial management on individual practitioners, who were forced to navigate complex social and economic dynamics. This period highlights a critical stage in the evolution of medical debt, in which the limitations of informal and credit-based systems became increasingly apparent. These challenges would eventually contribute to the development of more formalized and institutional approaches to healthcare payment in the modern era.
Informal Economies of Care: Sliding Scales and Social Obligation
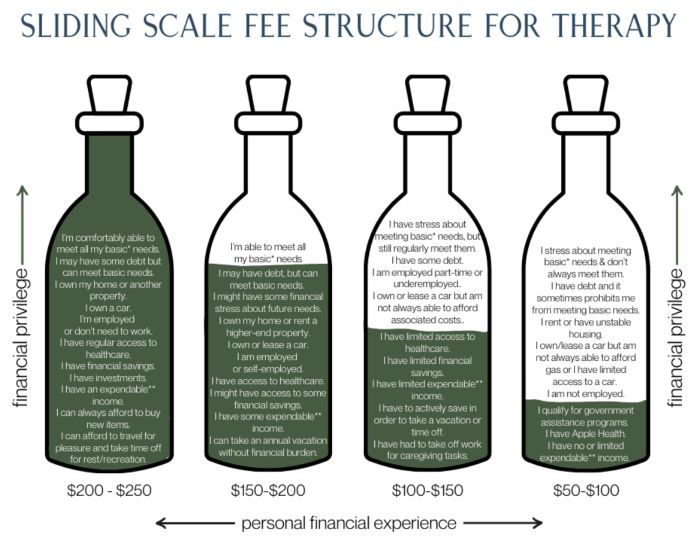
In the absence of standardized billing systems and institutionalized payment structures, premodern medical practice often relied on informal economies that blended financial exchange with social obligation. Physicians did not operate within rigid fee schedules but instead adjusted their charges according to the circumstances of each patient, taking into account factors such as wealth, status, and the nature of the illness. This flexibility allowed practitioners to navigate economic inequality while maintaining their livelihoods, creating a system in which payment was shaped as much by social relationships as by market principles. In many cases, the expectation of eventual compensation was sufficient to sustain the exchange, even if payment was delayed or incomplete. Medical debt was not always a fixed obligation but a negotiable and evolving aspect of the physician–patient relationship, reflecting the broader dynamics of trust and reciprocity that defined premodern communities.
The use of sliding-scale fees was one of the most common mechanisms through which physicians adapted to these conditions. Wealthier patients were typically charged higher fees, reflecting both their ability to pay and the expectation that they would subsidize care for others within the community. This practice allowed physicians to maintain a degree of financial stability while also fulfilling social and ethical expectations to provide care more broadly. In contrast, poorer patients might receive reduced-cost treatment or, in some cases, no charge at all, particularly in situations where the physician recognized the long-term value of maintaining goodwill or social standing. These arrangements were not always formalized but were instead shaped through negotiation and mutual understanding, often influenced by local customs and personal relationships. While this approach created opportunities for flexibility and inclusivity, it also reinforced existing social hierarchies, as access to the most skilled practitioners and advanced treatments often remained tied to wealth and status.
Barter and non-monetary exchange further illustrate the flexibility of these informal systems. In many communities, particularly those with limited access to currency, patients compensated physicians with goods, labor, or services. Payment might take the form of agricultural products, household items, or assistance with work, reflecting the localized nature of economic exchange. These arrangements allowed medical practice to function within economies that were not fully monetized, but they also introduced variability and uncertainty into the valuation of services. The worth of medical care was negotiated not only in financial terms but within the broader context of community exchange.
Social obligation played a central role in sustaining these informal economies, shaping expectations on both sides of the physician–patient relationship. Physicians were often expected to provide care regardless of immediate payment, particularly in cases of severe illness or among vulnerable populations, reinforcing the ethical dimension of medical practice. Patients were expected to fulfill their obligations when possible, whether through delayed payment or reciprocal support, creating a system in which debts could persist over extended periods without formal enforcement. Reputation functioned as a critical mechanism of accountability, as both practitioners and patients relied on their standing within the community to maintain trust and cooperation. A physician known for generosity might attract more patients, while one perceived as overly rigid in demanding payment risked social isolation. These dynamics created a system in which economic and moral considerations were deeply intertwined, ensuring that financial exchange remained embedded within broader patterns of social interaction.
Informal economies of care highlight the adaptability of medical practice in the face of economic constraints and social complexity. While these systems allowed for flexibility and responsiveness to individual circumstances, they also placed significant burdens on practitioners, who bore the risk of inconsistent or incomplete payment. The reliance on social obligation and negotiated exchange underscores the absence of formal enforcement mechanisms, revealing a model of medical debt that was fluid rather than fixed. This approach reflects a broader historical pattern in which healthcare functioned within a moral economy, balancing the demands of livelihood with the imperative to heal.
Legal and Ethical Tensions: Care vs. Compensation

The relationship between medical care and compensation has long been shaped by a fundamental tension between legal obligation and ethical duty. Physicians were expected to sustain themselves financially, yet they also operated within moral frameworks that emphasized the importance of healing regardless of a patient’s ability to pay. This dual expectation created an inherent contradiction, as the act of pursuing payment could conflict with the ideal of the physician as a compassionate caregiver. In premodern societies, where formal systems of billing and enforcement were limited, this tension was not resolved through institutional mechanisms but was instead negotiated on a case-by-case basis.
Legal systems provided some avenues for physicians to recover unpaid debts, but these mechanisms were often constrained by social and professional considerations. While courts could adjudicate disputes over fees, the process of pursuing legal action was not always practical or desirable. Physicians risked damaging their reputations if they were perceived as prioritizing profit over care, particularly in communities where personal relationships were central to professional success. In addition, legal proceedings could be costly, time-consuming, and uncertain in outcome, further discouraging practitioners from pursuing formal enforcement. Even when physicians succeeded in obtaining judgments, the actual recovery of payment could remain difficult, especially if patients lacked sufficient resources. Many practitioners weighed the potential benefits of legal action against the broader risks to their social standing and professional relationships, often concluding that informal negotiation or partial loss was preferable to aggressive enforcement.
Ethical frameworks within medicine further complicated the issue of compensation, as professional ideals emphasized duty, charity, and the preservation of life. Medical texts and traditions often encouraged physicians to treat the poor without expectation of immediate payment, framing such actions as both morally virtuous and professionally appropriate. These ideals did not eliminate the practical necessity of earning a living, leaving physicians to balance competing priorities. This balance was rarely stable, as economic pressures could conflict with ethical expectations, creating ongoing tension within the practice of medicine.
The ambiguity surrounding medical payment also extended to questions of value and outcome. Unlike many other forms of labor, the results of medical treatment were uncertain, and success could not be guaranteed. Patients might resist payment if treatment failed, while physicians argued that their expertise and effort merited compensation regardless of the outcome. This disagreement reflects a deeper issue in the valuation of medical services, where the intangible nature of knowledge and skill complicated the process of assigning monetary worth. In some cases, payment arrangements were explicitly tied to outcomes, while in others they were based on the time, effort, or reputation of the practitioner, leading to further inconsistency in expectations. These disputes reveal how the lack of standardized measures for evaluating medical success created fertile ground for conflict, as both patients and physicians operated with differing assumptions about what constituted fair compensation.
The tension between care and compensation reveals a persistent challenge at the heart of medical practice in the premodern world. Physicians operated within systems that demanded both economic sustainability and moral responsibility, often without clear guidance on how to reconcile the two. The resulting ambiguity shaped not only the management of medical debt but also the broader identity of the profession, as practitioners navigated the competing demands of livelihood and duty. This enduring conflict underscores the complexity of medical economics and its deep roots in historical practice.
Transition to Modern Systems: The Rise of Third-Party Payment

The transition from premodern systems of medical payment to modern, institutionalized frameworks represents a profound shift in how healthcare and debt were structured and managed. For centuries, the physician–patient relationship functioned as a largely direct and personal economic exchange, shaped by negotiation, reputation, and social obligation. By the mid-twentieth century, this model began to give way to systems in which payment was mediated by external institutions, particularly insurance companies. This transformation altered not only the mechanics of payment but also the nature of medical debt itself, moving it from a personal obligation to a more formalized and impersonal financial arrangement.
The rise of third-party payment systems was closely tied to broader economic and social developments, including industrialization, urbanization, and the expansion of wage labor. As populations became more mobile and less embedded in tightly knit local communities, the informal mechanisms that had previously governed medical payment became less effective. Patients were no longer consistently treated by long-standing family physicians within stable social networks, weakening the reciprocal obligations that had once underpinned flexible payment arrangements. The increasing cost and complexity of medical care created a demand for systems that could distribute financial risk more broadly. Hospitals expanded, new technologies emerged, and treatments became more specialized, all of which drove up costs beyond what many individuals could pay out of pocket. Early forms of health insurance, often organized through employers, fraternal organizations, or mutual aid societies, began to address this need by pooling resources and covering medical expenses on behalf of individuals, marking a critical step toward institutionalized payment systems.
The expansion of insurance systems after World War II marked a decisive turning point in the evolution of medical payment. In the United States, the growth of employer-sponsored health insurance fundamentally reshaped the economic landscape of healthcare, reducing the reliance on direct payment between patient and physician. Wartime wage controls had encouraged employers to offer health benefits as a form of compensation, and this practice continued in the postwar period, rapidly expanding coverage across the workforce. Hospitals and medical providers increasingly billed insurance companies rather than patients, introducing new layers of administration and standardization into the process. This shift not only stabilized revenue for providers but also distanced patients from the immediate financial implications of care, creating a system in which the true cost of treatment was often obscured. This separation between service and payment would have lasting consequences for both healthcare pricing and patient expectations.
The involvement of third parties introduced new forms of complexity and control into the healthcare system. Insurance companies developed standardized fee schedules, reimbursement policies, and eligibility criteria, which influenced both the cost and delivery of medical services. Physicians and hospitals were required to navigate these systems, often adjusting their practices to align with insurance requirements. While these changes brought greater consistency and predictability to payment, they also reduced the autonomy of practitioners and introduced bureaucratic constraints that had not been present in earlier periods.
The emergence of third-party payment systems also laid the groundwork for the development of modern medical debt as a distinct phenomenon. As healthcare costs continued to rise, gaps in coverage, deductibles, and exclusions created situations in which patients remained financially responsible for significant portions of their care. Unlike the informal debts of earlier periods, these obligations were increasingly subject to formal collection processes, including the involvement of specialized agencies. The personal, negotiated nature of medical debt gave way to standardized billing and enforcement mechanisms, transforming the experience of debt from a social relationship into a financial transaction governed by institutional rules.
The transition to modern systems of medical payment reflects a broader shift from localized, relationship-based economies to centralized and bureaucratic structures. While these systems addressed many of the limitations of earlier models, including the unpredictability of payment and the burden placed on individual practitioners, they also introduced new challenges related to accessibility, complexity, and equity. Patients gained greater access to care through pooled risk and expanded coverage, but they also became entangled in systems that were often difficult to navigate and, at times, financially burdensome. The rise of third-party payment did not eliminate the tensions between care and compensation but reconfigured them within a new institutional framework, one that continues to shape the experience of medical debt in the contemporary world and raises enduring questions about responsibility, fairness, and the true cost of care.
Historiography: Interpreting Medical Debt across Time
Historians have increasingly turned their attention to the question of medical debt as a lens through which to examine broader economic, social, and ethical structures across time. Rather than treating unpaid medical bills as a purely modern phenomenon, scholars have emphasized the long continuity of financial tension embedded within healthcare systems. From ancient contractual obligations to early modern fee disputes and modern institutional billing, the persistence of medical debt reflects the enduring challenge of reconciling the cost of care with the moral imperative to heal. Historiography in this field situates medical debt within larger debates about economic exchange, social hierarchy, and the professional identity of physicians.
One major line of interpretation focuses on the embeddedness of medical debt within local and social relationships in premodern contexts. Scholars have argued that in ancient and medieval societies, medical payment was inseparable from systems of patronage, reciprocity, and community obligation. In this view, debt was not simply a financial liability but part of a broader social negotiation, often mediated by reputation, status, and long-term relationships. Physicians operated within networks that allowed for flexibility in payment, including delayed compensation, in-kind exchanges, or the expectation of future services. This interpretation highlights the fundamentally relational nature of medical debt prior to the emergence of formalized financial systems.
A contrasting historiographical perspective emphasizes the gradual shift from these embedded systems to more formalized and impersonal structures of economic exchange. Historians have traced the transformation of medical practice in the modern era, arguing that the rise of hospitals, professionalization, and insurance systems fundamentally altered the nature of medical debt. This shift, they contend, marked the transition from a negotiated and socially mediated form of obligation to a standardized and bureaucratically enforced system. The emergence of third-party payment and institutional billing not only changed how debts were collected but also redefined the relationship between patient and provider, distancing it from its earlier social foundations. In addition, this transformation introduced new forms of financial abstraction, where costs were mediated through codes, reimbursements, and administrative processes that obscured the direct connection between treatment and payment. Historians in this camp often emphasize that this shift was not merely administrative but cultural, reshaping expectations about entitlement, responsibility, and the role of the state and private institutions in healthcare provision.
Another strand of scholarship explores the ethical dimensions of medical debt, particularly the tension between care and compensation. Historians of medicine have examined how physicians navigated the competing demands of professional livelihood and moral duty. This work underscores the persistent ambiguity surrounding medical payment, as practitioners were expected to balance economic necessity with ethical expectations of charity and service. Historians in this tradition often emphasize continuity rather than rupture, arguing that while the mechanisms of payment have changed, the underlying tension between financial sustainability and ethical obligation remains a defining feature of medical practice.
Finally, recent historiography has begun to connect the history of medical debt to contemporary debates about healthcare access and inequality. Scholars have drawn parallels between premodern practices of selective care, sliding scales, and informal negotiation and modern issues such as insurance gaps, medical bankruptcy, and the role of collection agencies. By situating current challenges within a longer historical trajectory, this body of work highlights both the persistence of inequality and the ways in which institutional frameworks shape the experience of debt. The historiographical evolution of this topic reflects a growing recognition that medical debt is not merely a byproduct of modern systems but a deeply rooted feature of healthcare across time.
Conclusion: The Long History of Medical Debt and Its Modern Implications
The history of medical debt reveals a persistent and evolving tension at the intersection of care, economics, and social obligation. From the formalized debt systems of ancient civilizations to the negotiated and community-based practices of the medieval and early modern periods, the challenge of compensating medical providers has never been fully resolved. What changes across time is not the existence of medical debt, but the structures through which it is created, managed, and enforced. These shifting frameworks reflect broader transformations in economic organization, legal systems, and the professionalization of medicine, demonstrating that medical debt is deeply embedded in the historical fabric of healthcare itself.
One of the most significant developments in this long trajectory is the gradual movement away from personal, relationship-based systems of payment toward impersonal, institutionalized mechanisms. In earlier periods, the physician–patient relationship was shaped by negotiation, reputation, and mutual obligation, allowing for flexibility in how debts were incurred and resolved. By contrast, modern systems of third-party payment and standardized billing have transformed medical debt into a more rigid and formalized financial obligation. This shift has brought greater consistency and scalability to healthcare systems, but it has also distanced patients from providers and introduced new forms of complexity that can obscure responsibility and accountability.
The ethical tensions that have long defined medical practice have not disappeared but have instead taken on new forms within modern systems. Physicians in earlier periods grappled with the balance between earning a livelihood and fulfilling their moral duty to treat the sick, often resolving this tension through informal accommodations or acts of charity. Today, similar questions arise within institutional frameworks, where issues such as insurance coverage, access to care, and the role of profit in healthcare continue to generate debate. The persistence of these ethical dilemmas underscores the continuity between past and present, suggesting that technological and organizational advances have not eliminated the fundamental challenges of medical economics.
The long history of medical debt provides critical insight into contemporary discussions about healthcare access, affordability, and justice. By situating modern practices within a broader historical context, it becomes clear that current systems are the product of centuries of negotiation between competing priorities. Understanding this history allows for a more nuanced evaluation of present-day challenges, highlighting both the progress that has been made and the enduring limitations that remain. Medical debt, far from being a uniquely modern problem, is a reflection of the ongoing effort to reconcile the human need for care with the economic realities that sustain it.
Bibliography
- Digby, Anne. Making a Medical Living: Doctors and Patients in the English Market for Medicine, 1720–1911. Cambridge: Cambridge University Press, 1994.
- Hammond, E. A. “Incomes of Medieval English Doctors.” Journal of the History of Medicine and Allied Sciences 15:2 (1960), 154-169.
- Hoffman, Beatrix. Health Care for Some: Rights and Rationing in the United States since 1930. Chicago: University of Chicago Press, 2012.
- Johnston, David. Roman Law in Context. Cambridge: Cambridge University Press, 1999.
- Jouanna, Jacques. Hippocrates. Translated by M. B. DeBevoise. Baltimore: Johns Hopkins University Press, 1999.
- Messac, Luke. “Debt Collection in American Medicine — A History.” The New England Journal of Medicine 389:17 (2023), 1621-1625.
- Messac, Luke, Blake N. Shultz, and Ahmed M. Ahmed. “Medical Debt in America, Part III: Debt Collection.” Journal of Hospital Medicine 20:7 (2025), 784-786.
- Numbers, Ronald L., ed. Medicine in the New World: Native Healing, Colonial Medicine, and the Emergence of American Medical Practice. Knoxville: University of Tennessee Press, 1987.
- Nutton, Vivian. Ancient Medicine. 2nd ed. London: Routledge, 2012.
- Pace, Brian P. “Ancient Medical Fees.” Journal of the American Medical Association 280:12 (1998).
- Park, Katharine. Doctors and Medicine in Early Renaissance Florence. Princeton: Princeton University Press, 1985.
- Porter, Roy. The Greatest Benefit to Mankind: A Medical History of Humanity. New York: W. W. Norton, 1997.
- Rawcliffe, Carole. Medicine and Society in Later Medieval England. Stroud: Sutton Publishing, 1995.
- Riddle, John M. A History of the Middle Ages, 300–1500. Lanham: Rowman & Littlefield, 2008.
- Risse, Guenter B. Mending Bodies, Saving Souls: A History of Hospitals. New York: Oxford University Press, 1999.
- Rosenberg, Charles E. The Care of Strangers: The Rise of America’s Hospital System. New York: Basic Books, 1987.
- Roth, Martha T., trans. Law Collections from Mesopotamia and Asia Minor. 2nd ed. Atlanta: Scholars Press, 1997.
- Siraisi, Nancy G. Medieval and Early Renaissance Medicine: An Introduction to Knowledge and Practice. Chicago: University of Chicago Press, 1990.
- Starr, Paul. The Social Transformation of American Medicine. New York: Basic Books, 1982.
- Temkin, Owsei. Hippocrates in a World of Pagans and Christians. Baltimore: Johns Hopkins University Press, 1991.
Originally published by Brewminate, 04.02.2026, under the terms of a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International license.


