In 2005, Dr. Terrence Tumpey, a Center for Disease Control Microbiologist, examines recreated 1918 Pandemic Influenza Virus to help understand its particularly deadly effects. By studying past pandemics, and the successes and failures of social and medical responses to end them, policy-makers and scientists hope to ameliorate the ill effects of the next flu pandemic before it begins.
By Dr. Anne Sealey
Policy Advisor at Ontario Public Service
The Ohio State University
In the spring of 2003 I collapsed at a college debating tournament dinner and soon found myself in quarantine in Guelph, Ontario. Collapsing with a cough and fever is worrisome at any time. It was particularly troubling to me and to the intake nurse who whisked me into an isolated room because at the time I was living in Toronto, which was then one of several cities internationally caught in the grip of a frightening new respiratory disease. SARS, Severe Acute Respiratory Syndrome, was a viral lung infection that caused atypical pneumonia and was frequently fatal.
In my case, the ER doctor determined that I had a less serious virus and mild exhaustion, and released me from my HEPA-filter prison. Other patients weren’t so lucky. Worldwide, SARS killed an estimated 774 of the 8,096 people infected, a fatality rate of 9.6%. The world, all things considered, was fortunate. While those deaths were tragic, they were a fraction of what was feared.
The signs in 2003 had been ominous for those familiar with medical history. SARS produced pneumonia in otherwise healthy adults, turning them blue before leaving them to drown in their own lung fluids. The threat of a pandemic felt very real.
Although SARS is a different type of virus, such frightening symptoms brought to mind one of the greatest public health nightmares of the twentieth century: the influenza pandemic of 1918-1919, the most widespread and fatal in recorded history. That pandemic of the influenza A virus killed anywhere from 50 to 100 million people worldwide, many of whom were young and healthy before being stricken. It caused widespread social and economic upheaval, and SARS looked poised to potentially do the same.
In the end, SARS was not contagious enough to cause such widespread devastation. Yet, since the SARS outbreak, the world has remained on high alert, watching nervously for a new pandemic, whether flu or some other respiratory disease.
Beginning in 2004, Asian “Bird Flu,” H5N1, a deadly form of influenza, attracted much anxious attention. But, as we soon learned, the concern was misdirected. The next pandemic came not from birds but from swine and, for Americans, from much closer to home.
In spring of 2009, reports of a particularly deadly form of influenza A—H1N1—began appearing in Mexico and the American southwest. By June, the World Health Organization announced that the disease had spread widely enough to be considered pandemic. The virus spread globally, peaking, it seems, in the later months of 2009 and causing over 14,000 deaths worldwide. What the world dodged in 2003 with SARS it could not in 2009. Pandemic influenza, a frequent visitor in the past, was back again.
As the threat of the H1N1 virus began to fade (for this year at least), the world breathed a sigh of relief that we had avoided a repeat of 1918. Yet, people around the globe continue to worry and wonder how best to prepare for, perhaps even prevent, the next pandemic.
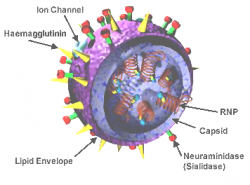
3D Model of an Influenza Virus. The Hemagglutinin (HA) and Neuraminidase (NA) proteins are shown on the surface, and are used to describe different types of Influenza viruses
The viruses that affect humans come in many types, and their impact on human communities varies considerably according to the qualities of a particular virus—how contagious and how virulent or fatal—and the ways that human societies act or structure themselves that facilitate (or block) a virus’s spread.
SARS and influenza hold a special place in pandemic planning because, like any airborne virus, they can be caught from casual contact: from a sneeze on a bus, a dirty door handle, or a shared water fountain.
Although viruses such as Ebola—which causes bleeding from the eyes, mouth, and organs—are deadlier, they require more direct contact to be transmitted and, with proper local quarantines, usually burn themselves out before they can spread.
Likewise, HIV, the virus that causes AIDS, has been pandemic for decades. HIV, however, is more difficult to transmit than airborne influenza or SARS, and requires different community-based initiatives for its treatment and prevention. The stigma that has long been associated with HIV has also allowed many to ignore the disease (at their peril) as one that happens to other people.
While diseases such as HIV and Ebola brought viruses back into the consciousness of the Western public, long accustomed to the safety afforded by antibiotics and vaccines, they represent a different public health danger than influenza and SARS.
Influenza is one of humanity’s most persistent and constant foes—many will get sick each year with some form of flu, some of them will die—but only every so often does a pandemic occur. While it is impossible to prevent influenza, today we are working to reduce the chance of a pandemic and we are learning how to respond more efficiently to pandemics when they hit to avoid mass fatalities.
Influenza, unlike some epidemic diseases, has no magic bullet. As a virus, it is impervious to antibiotics. Anti-virals can help, but they do not cure. So influenza, like many viral illnesses, requires an array of strategies to deal with infection and containment. And it requires no small amount of luck. A century of advancing medical science has given humanity a variety of new weapons to fight the spread of influenza. But each has its limitations.
Going forward, to minimize or avoid the next pandemic, humans need to understand fully the patterns of human and viral behavior, and to look not only to cataclysmic pandemics like 1918 for lessons but also to the less spectacular flu pandemics that have dotted the landscape of the twentieth century.
A Very Brief History of Pandemic Influenza
The Oakland Municipal Auditorium in use as a temporary hospital during the 1918 flu epidemic. Here, volunteer nurses from the American Red Cross are tending the sick
Influenza is a perpetual scourge. Even though its fatality rate is relatively low (typically 0.1% deaths per infected individual), in an average year, influenza kills 250,000 to 500,000 globally according to a 2003 World Health Organization (WHO) estimate. In America, 98,000 can expect to be hospitalized, and there are, on average, 36,000 deaths, of which 82 are children. By contrast, cancer kills 500,000 Americans annually and car crashes kill 42,000.
Pandemic influenza is far deadlier. Pandemics, according to the current WHO definition, are new viruses that spread quickly, human to human, over a broad geographic area, taking advantage of a lack of prior immunity. In the popular understanding, pandemics are also considered especially sickening or deadly. (Until recently, this was approximately the way the WHO classified them as well.) In 1918, approximately 675,000 Americans lost their lives to influenza. In 2009, approximately, 8,000-16,000 Americans have died, and perhaps 60 million Americans have been sickened.
Pandemic influenza has a long history. In the 1600s, “Sweating sickness” panicked Europe, spreading in towns and royal courts across the continent. Later, similar diseases earned the name influenza—from the Italian word for influence—because they travelled so quickly that people reasoned the only way so many could become so ill so fast was if poor weather conditions or astrological forces were the cause.
The first “modern” pandemic occurred in 1890 and was called the Russian flu, because it was believed to have originated in Siberia. With new technologies like the steamship and the railway, diseases like influenza had easier ways to spread over long distances. A journey for disease that would have taken months from Moscow to London when people traveled by foot, boat, or cart, now took mere weeks, giving populations less time to prepare and less opportunity to quarantine. Luckily, the “Russian flu” was fairly mild. While many became ill, relatively few died.
“The mother of all” influenza pandemics took place in 1918, and the memory of it continues to strike the most fear into the heart of medical professionals and historians alike. In the midst of the chaos, hardship, and human displacement of World War I, an unusually deadly strain of influenza began to emerge in the spring. By the fall, after a brief lull in the outbreak, the full force of the virus began to hit. An estimated one third of the world’s population were infected and showed symptoms of the illness.
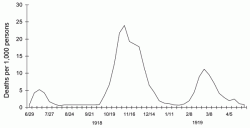
Chart showing the three pandemic waves in 1918-1919 through weekly combined influenza and pneumonia mortality, United Kingdom
“Black Octobers” and “Black Novembers” greeted many countries, when the second wave’s death toll was highest. At its worst, the pandemic brought cities to their knees. Patients who were healthy one day were “gripped” by fever the next, experiencing difficulty breathing and muscle weakness. By the end of the pandemic, between 50 and 100 million people worldwide had turned blue and died (a rate of approximately 2.5% case-fatality). Gymnasiums were turned into morgues when too many died to fit into hospitals or cemeteries.
No one is quite sure why the 1918 pandemic turned out so badly. With World War I still raging, people in Europe were hungry and stretched to the breaking point, making them more susceptible to infection. Peace-time social services were no longer operating and many people lived in crowded and unsanitary conditions. Troops, migrant laborers, and refugees spread the virus rapidly across vast distances.
Even the end of the war had its dangers. When the Armistice was signed in November, 1918 many communities saw an uptick in flu cases as happy and relieved citizens celebrated together, sharing good wishes and influenza at parades and parties. A third, less deadly wave appeared in the spring before the epidemic died down in mid-1919.
After 1918, the world had a chance to catch its breath. In fact, the severity of 1918 seemed to provide some immunity against later infections, for a little while at least. In 1957-1958 and 1968-1969, however, there were two “minor” pandemics—minor at least when compared to 1918.
The 1957 pandemic began in Guizhou, China, then spread to Singapore, Hong Kong and moved into the United States by the fall, where it killed an estimated 70,000 people. Total deaths globally were between 1.5 to 2 million people.
Many people in 1957 still remembered the 1918 pandemic and were on edge. In an effort to avoid panic, the publication of a book commemorating the fortieth anniversary of the 1918 pandemic, called “Invasion by Virus: Can it Happen Again?” was delayed when the answer had clearly become “yes.”
In 1968, another virus began, we think, in Asia. The “Hong Kong flu” was marked by high morbidity but relatively low fatality—that is, many got sick but few died. Only 34,000 Americans were killed and an estimated one million worldwide. Many older people were unaffected, probably because they had caught and survived the similar 1918 influenza.
Despite the low death rates, such frequent flu pandemics have made the world anxious. In 1976, when swine flu was detected at Fort Dix Army Base in New Jersey, health officials sounded the alarm. The 1918 pandemic had been a swine flu as well, and they worried that after the “near misses” of 1957 and 1968 that the world was due for another nightmarish pandemic. That pandemic didn’t materialize, but it did generate a large-scale American vaccine program, which has shaped many our modern anti-influenza measures.
Modern Responses
Death tolls for the present pandemic are mercifully lower than for 1918. It seems, perhaps, that the virus is less lethal. There is no world war that has weakened the population and basic sanitary situations have improved in many parts of the world. Thanks to a century of medical research, we have better respirators, anti-virals and vaccines that treat or prevent influenza directly. We also have antibiotics that, with luck, help to counteract the bacterial “purulent bronchitis”—a form of pneumonia that develops in the fluid in the lungs of an influenza sufferer—that carried away many of 1918’s victims.
There is some hope that a massive pandemic like 1918 might be avoided in the future with well-conceived counter-measures, prevention, and some good fortune.
In the most recent pandemic, three levels of prevention were used: first, an international surveillance system at the global level; second, a system of pre-emptive vaccination; and finally, an emphasis on personal prevention. But each of these tools has benefits and drawbacks, which are exacerbated by human error or misunderstandings. In 2009, humans around the planet made mistakes in judgment that are eerily familiar to problems in past anti-influenza campaigns and helped to spread the virus.
Global Influenza Monitoring
Chart showing the “W Curve” of Spanish Flu mortality, which disproportionally affected healthy young adults
The worldwide system for determining and monitoring pandemics is a relatively recent invention. In 1918 there was no planet-wide health organization like the WHO, and, while there were radios and telegraphs to spread information, there was no CNN to report its findings to a waiting world or obviously no internet. The only international system for coordinating disease, the Paris-based International Public Health Office, was all but shut down as a result of World War I.
To make matters worse, the war slowed down the spread of crucial information about the disease in other ways. Anxious to avoid giving away potential military advantage, states involved in World War I refused to release flu data. This is why the 1918 pandemic was referred to as the Spanish Flu. Spain didn’t participate in World War I, so it published its disease statistics internationally while other nations did not.
In the 1950s, the WHO adopted the pandemic influenza warning system that had been developed informally in the 1940s amongst doctors who had lived through the 1918 pandemic. The WHO early warning system effectively picked up on the 1957 and 1968 pandemics before they spread, which helped to prevent a devastating flu pandemic.
The Centers for Disease Control and Prevention Headquarters in DeKalb County, GA
Today, the WHO and national epidemiological intelligence centers such as the Centers for Disease Control and Prevention (CDC) in Atlanta, as well as a network including more than 100 laboratories worldwide, coordinate the epidemiological data that makes declaring a pandemic possible.
They also centrally determine what strands of vaccine should be prepared, manufactured, and shipped around the world in a complicated web of international, national, not-for-profit, and commercial organizations. Although the WHO determines the strains that should be included in the vaccine, production and approval is left to the appropriate national or regional drug-approval body.
This early warning system has become vital to influenza control efforts even if it has sometimes led to false-positives, such as in 1976 and the recent attention to H5N1 Avian flu. The overlap between national and international bodies, however, has complicated a number of key steps in anti-influenza campaigns, most notably vaccine production.
Vaccines
President Barack Obama receives an H1N1 vaccine during the 2009 H1N1 Pandemic, December 2009
Vaccines have become another standard first line of defense against seasonal flu.
In 1933, a ferret in a British medical lab sneezed on a researcher infecting him with flu. While the scientist was likely not pleased to be infected, it was a great moment in medicine because it established that viruses were responsible for human influenza.
Until then, the world had assumed that flu was caused by a bacterium discovered by German scientist Richard Friedrich Johannes Pfeiffer at the end of the 1890 pandemic. Flu vaccines targeted this bacterium in the early twentieth century. However, faith in Pfeiffer’s bacillus did not survive the 1918 pandemic. His vaccines simply did not stop the disease.
After 1918, many scientists came to believe that the flu was caused by a so-called “filter passing virus.” Their belief was backed up by the fact that when examined, the secretions of influenza patients did not contain a common organism that seemed to be causing the disease. Thus, they reasoned, the disease must be caused by something smaller that they could not catch. An influenza virus was identified in pigs in 1931, but not in humans until that fateful, snotty-nosed-ferret day in 1933.
With the virus found, a vaccine was in reach. Soldiers in World War II were among the first to receive the new vaccine, as military planners feared that the Second World War might bring with it an influenza pandemic like the previous world war. In fact, the egg technology used today to produce influenza vaccines dates to the 1950s.
In the 1957 and 1968 pandemics, public vaccine programs were in their infancy. Just 15-20 million doses of vaccine were made annually in the United States. Only 8-12 million American civilians were annually vaccinated, which meant that there was no capacity to easily and quickly vaccinate large numbers of people, either in the United States or around the world.
With the early warning provided by the WHO in 1957, however, the American government decided to gear up to vaccinate more widely. Negotiations with vaccine producers immediately proved difficult. They were hesitant to produce an expensive product when there was no proof the pandemic would reach the U.S. When they at last agreed to make the vaccines—because evidence could no longer be ignored that the pandemic had indeed grown—it was essentially too late.
Although the U.S. managed to vaccinate a larger percentage of the population than ever before, it was only after a period of panic that there would not be enough available. With vaccine production starting late in the game, the American vaccination program also came at the cost of many unused vials of vaccine that came off the production lines after the pandemic had essentially passed. Not much was learned from these experiences and a similar pattern of events occurred in 1968.
Then came the 1976 swine flu scare. With the makings of another swine flu pandemic, the American government authorized the National Influenza Inoculation Program. The program seemed cursed from the beginning. The country lacked the ability to produce the vaccine in the requisite quantities, and what it did produce appeared to cause serious neurological problems in a small number of patients. Panic ensued.
Today, it is unclear whether there was in fact any link between the symptoms and vaccine, but the incident prompted tremendous concern at the time. Only 30% of the population was vaccinated despite hopes that upwards of 90% would be. Even after more than a quarter century of safe vaccine, mass vaccination rates still hover at about where they were in 1976, at around 30% of the population.
This year, a similar series of events unfolded. The strain of influenza that turned pandemic was not mixed into the seasonal flu vaccine because it was not seen as a threat at the time vaccines were being produced. Few people had been sickened by H1N1 when the decision was made over what would go into the seasonal flu vaccine cocktail, and experts still focused their attention on the Avian strains. Once it became clear that the 2009 H1N1 virus was likely to spread, there was a scramble for vaccine. Alarm broke out in many regions as the vaccine remained scarce, and calls of queue jumping were common when hockey players, Wall Street moguls, and politicians seemed to get the limited vaccine before the rest of us.
By early 2010, there was excess vaccine in many places where there had been a shortage earlier. France and Canada are looking to sell theirs to a world that may no longer need it, repeating the mistakes of the past. The current version will offer limited protection next year, given that many have already had the disease and other flu viruses will evolve for the next season, making the single strain vaccine developed on the fly this year too little, too late.
Local Measures
Street car conductor in Seattle not allowing passengers aboard without a mask, 1918
Despite the advances (and institutional difficulties) of monitoring systems and vaccines, one of the best preventive steps against the spread of flu was and still is to change human ‘s weave was actually too loose to trap the virus. Modern paper and cloth masks are much more effective. A study reported on in the Annals of Internal Medicine found that family members of influenza patients drastically cut their risk of infection if they wore masks and washed their hands regularly.
Finally, public education campaigns have focused on having people change their day-to-day habits to limit the spread of the disease. Health campaigns to have people stop shaking hands or hugging when greeting met with limited success. Yet, many more people responded to suggestions to sneeze or cough into a sleeve rather than the hand, to prevent transferring viruses to other people.
Lessons Learned and Future Pandemics?
The twentieth century was largely one of triumph for medical science. Antibiotics were discovered, and innumerable life-saving therapies developed. In the west, we have the privilege to think that we are, for the most part, immune from contagious diseases.
The influenza outbreak challenges this hard-won privilege. The flu virus remains, despite the best efforts of medical and public health professionals, a difficult foe. At the beginning of the twenty-first century, we are almost as susceptible to it as we were 90 years ago, thanks to the convergence of biology, politics, technology, and individual action.
In late March, the CDC held its first press conference on swine flu in months. A recent outbreak in Georgia had left 40 people hospitalized and the CDC believed it was a result of vaccination problems. Unlike in the past, however, in this instance, vaccine was readily available. Many of those hospitalized, along with the majority of American adults, had simply chosen not to take the vaccine offered, despite the fact the CDC estimated that there were 140 million excess doses available by early 2010.
It is too early to say why many adults have not received the vaccine. Was it poor publicity of the availability of the vaccine following the early shortages? Were the vaccines not covered by insurance plans or otherwise unaffordable? Did they have underlying health problems that made taking the vaccine ill-advised? Or were they part of a growing movement of vaccine refusal?
In the European Union, some accused the WHO of declaring a pandemic to line the pockets of vaccine manufacturers. Others maintained, despite all evidence to the contrary, that the vaccine was unsafe, tapping into older anti-vaccine feelings. In the United States, a growing number of adults are regularly refusing vaccines, resulting in an estimated extra 50,000 deaths annually from pneumonia, influenza and other diseases.
As with influenza vaccines, there are few controls or mechanisms for vaccinating adults. Most successful vaccination campaigns—such as the MMR vaccine or polio in years gone by—are conducted on infants or school children. How to distribute vaccine is a complicated technological, administrative, political, medical, and social problem.
This latest influenza outbreak highlights the unpredictability of flu epidemics, and the complexity of the problem to be solved. While medicine and science traditionally look forward, the messy social and political problems inherent in defending ourselves against epidemics suggest that looking back to appreciate that epidemics are not just medical but administrative problems would help us plan better.
Because one thing is certain: there will always be another flu season.
Suggested Reading
Beveridge, WIB. “The Chronicle of Influenza Epidemics.” History and Philosophy of the Life Sciences 13, no. 2 (1991): 223-235.
CDC. “CDC Estimates of 2009 H1N1 Influenza Cases, Hospitalizations and Deaths in the United States, April – December 12, 2009.” http://cdc.gov/h1n1flu/estimates_2009_h1n1.htm [Accessed January 25, 2010].
Collier, Richard. The Plague of the Spanish Lady: The Influenza Pandemic of 1918-1919. New york: Atheneum, 1974.
Crosby, Alfred W. American’s Forgotten Pandemic: The Influenza of 1918. Cambridge: Cambridge University Press, 1989.
Davis, Mike. The Monster at our Door: the Global Threat of Avian Flu. New York: The New Press, 2005.
Graves, Charles. Invasion by Virus: can it happen again? London: Icon Books, 1969.
Honigsbaum, Mark. Living with Enza: The Forgotten Story of Britain and the Great Flu Pandemic of 1918. Hampshire: Macmillan Science, 2008.
Johnson, Niall P. A. S., and Juergen Mueller. “Updating the Accounts: Global Mortality of the 1918-1920 ‘Spanish’ Influenza Pandemic.” Bulletin of the History of Medicine 76 (2002): 105-115.
Neustadt, Richard E. and Harvey V. Fineberg. The Epidemic that never Was: Policy-Making and the Swine Flu Scare. New York: Vintage Books: 1982.
Patterson, K. David. Pandemic Influenza 1700-1900: A Study in Historical Epidemiology. Totowa, NJ: Rowman & Littlefield, 1986.
Pettit, Dorothy A. and Janice Bailie, A Cruel Wind: Pandemic Flu in America, 1918-1920. Murfreesboro: Timberlane Books, 2008.
Phillips, Howard and David Killingray, The Spanish Influenza Pandemic of 1918-19: New Perspectives. London: Routledge, 2003.
Rice, Geoffrey W with assistance from Linda Dryder. Black November: The 1918 Influenza Pandemic in New Zealand. 2nd ed. Christchurch, New Zealand: Canterbury University Press, 2005.
Silverstein, Arthur M. Pure Politics and Impure Science: The Swine Flu Affair. Baltimore: The Johns Hopkins University Press, 1981.
Originally published by Origins: Current Events in Historical Perspective (Vol. 3, Issue 8, May 2010) history departments of The Ohio State University and Miami University, under a Creative Commons license.